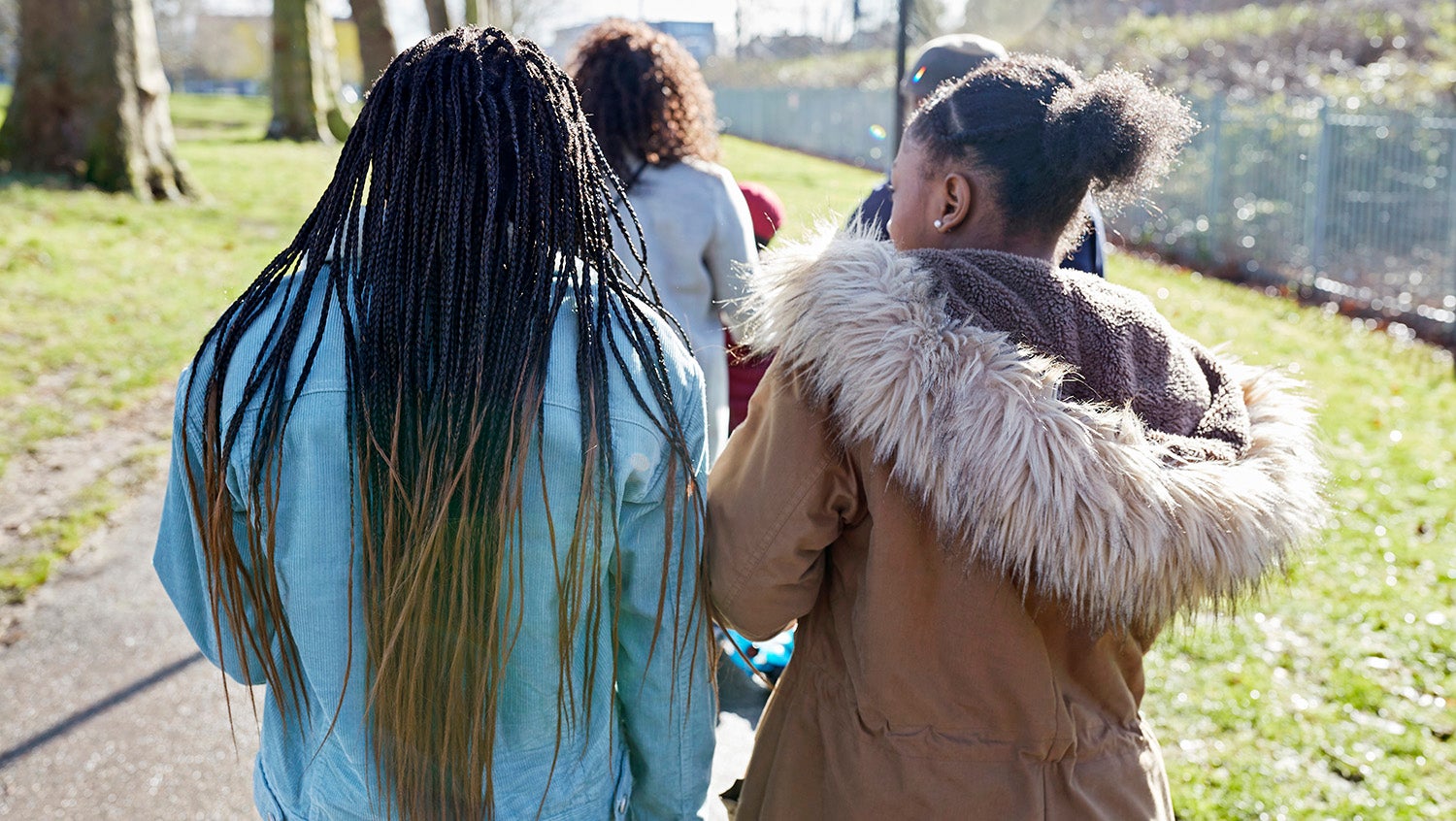
Getty Images
“We don’t ask young people what kind of program they might want or need, but we still expect them to come and engage in what we’re offering.”
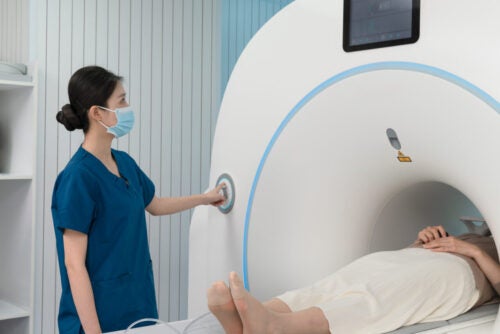
As a physician practicing family medicine, Katherine Gergen Barnett, MD, has seen many young patients brought in by their parents for checkups and preventative care through childhood and early adolescence, only to stop coming for appointments when they hit the high school and college years.
“What the literature shows us is that there’s a big drop-off in engagement,” she says. “I’m very curious about that: What are the barriers to engagement, and what are we doing as a system to enable them?”
While examining and boosting youth participation in care delivery systems can be challenging, she says, it may lead to greater health equity, better quality of care, and improved outcomes for accountable care organizations (ACOs) and other providers, ultimately reducing short- and long-term costs.
Healthcare and youth participation in action
An understanding of the top health concerns of young people and the hurdles to their seeking care is among the benefits of engaging teens and young adults in research, healthcare policy, and care transformation, says Gergen Barnett, who coauthored a recent study on youth engagement in Health Affairs. She serves as vice chair of primary care innovation and transformation and program director of family medicine at Boston Medical Center.
In the study, researchers recruited 12 local Black and Latinx youth ages 13 to 18 and hired a young adult facilitator to lead a community health assessment. Participants designed and conducted a community survey to understand their health concerns.
“They conducted a health assessment with their peers and other people in their community, and they were able to reach people we might not have otherwise heard from,” says Linda Sprague Martinez, PhD, lead author of the study and associate professor and department chair of macro practice at the Boston University School of Social Work.
Youth ultimately identified mental and sexual health, food access, and community safety as the community’s top health concerns, and developed recommendations for improving health and addressing inequities.
The project helped providers identify blind spots in existing care delivery systems, including some that surprised the researchers.
“One of the things the youth health assessment identified as a big barrier to health is access to behavioral health care,” says Gergen Barnett. “But we have a huge behavioral health arm of our services. We have social workers, we have psychiatrists, and there’s an innovative family medicine psychiatry program. In my mind, we have tons of access to behavioral health — so where’s the gap?”
The survey proved illuminating. Barriers identified by the survey included lack of transportation and cultural or generational differences, such as immigrant parents who have a more skeptical attitude toward mental health care than their American-born teens. But the biggest gap, according to teens, is awareness.
“You can have all the services in the world, but if young people don’t know about them it’s not going to be helpful,” Sprague Martinez says.
The benefit to accountable care organizations (ACOs)
It just makes sense that understanding the needs of young people and designing healthcare systems with them in mind can increase their participation and use of services, Sprague Martinez says: “If someone’s throwing a party for you, you would want to have a say in what kind of party it is and what would make you want to attend. In healthcare, we don’t ask them what kind of program they might want or need, but we still expect them to come and engage in what we’re offering.”
But ACOs and other healthcare providers have a big incentive to design healthcare systems in a way that will keep people engaged through their teens and 20s, which can lead to better health outcomes years and even decades down the road. Early screening and appropriate support for conditions such as depression, anxiety, diabetes, and hypertension can improve longevity and reduce the disease burden over the long term, Gergen Barnett says. And adolescents who engage with the healthcare system and build trusting relationships with providers are more likely to continue seeking preventive care over the course of their adult lives.
“There are certain places in a life course where there are real opportunities to make a health impact,” Gergen Barnett says, noting adolescence and young adulthood as one of them.
For ACOs, in addition to the cost savings of improved overall health, increasing youth participation can also improve performance on measurable criteria like total screenings for behavioral health or sexually transmitted infections, she notes.
Youth engagement in programs like the community health assessment survey can also help feed the workforce pipeline, increasing the number of Black, Latinx, and other youth of color entering healthcare careers, a key goal for healthcare organizations aiming to reflect the populations they serve, the authors say. Sprague Martinez shares that one of the young men in the project is now entering college and considering a career in public health or healthcare.
Increasing youth participation in healthcare development
But engaging young voices in healthcare development can be challenging. Concerns like transportation, lack of identification, and lack of a bank account to receive payment for their work can be barriers to youth participation in leadership roles. So can institutional culture, resistance to change, and lack of buy-in by adults within the organization who believe a young person can’t be an expert. Some organizations make the mistake of appointing a young person to serve on a board but fail to support their participation in a meaningful way, which can tokenize that young person, Sprague Martinez says.
Instead, healthcare institutions should start with an organizational assessment and identify where youth participation is possible, what staff would be involved, what systems are in place to support the process, and what training might be needed to prepare adult stakeholders to work collaboratively with youth in a way that is supportive of young people.
“I feel again and again that I am a complete beginner in this process, and I love it,” says Gergen Barnett. “This kind of work, especially where the youth who are engaged are not afraid to really push back and tell you their truths, it’s humbling.”