Special Pathogens Unit Nurses Are Already Preparing for the Next New Virus
August 3, 2021
By Meryl Bailey

Nahid Bhadelia
When COVID-19 hit Boston, it proved just how vital the SPU's trainings, outbreak simulations, and drills were. Nurses were ready to retool hospital procedures in response.
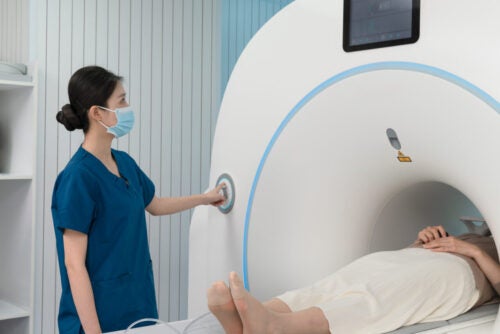
At first glimpse, the three rooms with railed beds in Boston Medical Center’s Menino building in a small alcove off floor 7 West look like any other hospital treatment areas. But the curious observer might notice slight differences that set the space apart. A glance underfoot will reveal the floor’s subtle progression from cool tones near the door to much warmer tones near the bed. A swivel of the head will show that the privacy blinds close between the glass panes on the doors. Scanning the walls above, a video camera and intercom system dot the corner near the ceiling.
This is Boston Medical Center’s Special Pathogens Unit (SPU), a state-of-the-art treatment space built to provide care for people who have been infected with the world’s most lethal emerging pathogens: hemorrhagic fevers like Ebola and Lassa and highly contagious respiratory infections like SARS-CoV and MERS-CoV.
How the special pathogens unit at Boston Medical Center works
Built in 2015, the SPU is a containment and treatment ward developed primarily to support researchers working at the nearby National Emerging Infectious Disease Laboratories (NEIDL), one of only two laboratories in the nation where researchers work to advance treatments for biosafety level 4 infectious agents, agents with a high mortality rate and no known cure. These researchers must don space-like positive-pressure suits before stepping through a series of containment rooms to look through a microscope. A researcher would be transported to BMC’s SPU for observation and care in the unlikely case of pathogen exposure.

Special pathogens unit team members in their PPE. (Nahid Bhadelia)
Every square inch of the SPU is designed to contain the spread of infection. The surfaces are poreless and seamless for easy sanitization and decontamination. The specially designed pressurized airflow system cleans the air through a series of filters. To answer the questions of the curious observer new to the SPU: The color progression on the floor? A reminder to caregivers about the increased level of infection as they near the patient’s bed. The video camera and intercom? Necessary for the buddy-system approach to care that ensures the safety of physicians and nurses treating patients.
Although BMC’s SPU supports researchers at the NEIDL, similar units dot the country in major city hospitals close to busy airports. Their strategic placement is the first line of defense to contain and treat sickened travelers suspected of harboring a contagious pathogen and hopefully to stop an outbreak before it occurs.

BMC’s Special Pathogens Unit trainings and simulation. (Nahid Bhadelia)
COVID-19 highlights the importance of preparedness
Preparedness to contain novel viruses is becoming more critical as the world’s population becomes increasingly mobile. Any part of the world is now reachable by plane in 36 hours, and an emerging infectious disease is recognized nearly every year. Many are zoonotic—meaning the infection makes the leap from an animal host to a human—and experts worry that habitat destruction and global climate change could accelerate the rate at which these events occur.
“It’s become even more important than ever that we build resilience against emerging infectious diseases threats so that we can keep our healthcare workers and our communities safe,” says Nahid Bhadelia, MD, then-medical director of the SPU, who helped found and build the program over the last 10 years, and associate director at NEIDL.

Nahid Bhadelia and members of the BMC SPU team. (Nahid Bhadelia)
One needn’t look at a calendar to remember how life-altering a viral pandemic can be. In December 2019, a new respiratory virus with zoonotic origin began circulating rapidly in Wuhan, China. When cases arrived in the United States in late January 2020, human-to-human transmission was already spreading in countries far beyond the capacity of all U.S. special pathogen units combined. The world is currently entrenched in chasing a rapidly mutating, highly contagious infection.
Bhadelia, who was just announced as the founding director of a new Boston University-wide center named the Center for Emerging Infectious Diseases Policy and Research (CEID), highlights how the SPU has served as will continue to serve as a critical partner in the effort to distribute best practices in containment care and training.
Nurses proved the power of SPU training
When COVID-19 arrived in Boston, the real power of the SPU was revealed, not within its sealed walls but in the legion of nurses the unit’s leadership train. At BMC, 115 nurses—including all the nurses from Menino 7 West and subgroups of intensive care unit and emergency department nurses—meet twice yearly for specialty training on all aspects of care highly communicable diseases. The simulations and drills prepare staff to rapidly engage if the unit activates. Still, as BMC’s nurse director of the SPU Kate Baudin, BSN, RN, explains, the infection containment procedures practiced during simulations had an incredible impact on the hospital’s response to COVID-19.

Nurses in the Special Pathogens Unit getting on their PPE. (Nahid Bhadelia)
“We hoped what we were training was effective, but you don’t really know, right? Because the hope is never to activate. When COVID came, our nurses were so well-prepared to manage containment of an unknown virus. They were able to get in and out of the PPE [personal protective equipment] effectively. They helped guide other hospital units to feel more comfortable in donning and doffing. They were key stakeholders in looking at procedures and saying, ‘this will work and this won’t,'” Baudin explains.
The rooms in Menino 7 West became BMC’s first dedicated COVID-19 treatment ward—a decision made in part because of the personnel’s specialty training. Nurses here had trained on SPU protocols for treating the highly infectious, including methods for lab draws, medication administration, intubation, and waste removal. Each procedure is refined to maximize a caregiver’s time with the patient before exiting the room and doffing the intricate layers of PPE.

BMC’s SPU team conducting a drill. (Nahid Bhadelia)
Navigating the influx of COVID-19 patients, nurses became integral problem-solvers in helping to retool hospital procedures to better serve the critically ill while protecting the hospital staff caring for them. Policies around trash removal, dietary trays, and phlebotomy all had to be redesigned. A simple procedure like monitoring glucose levels and administering insulin in diabetic patients, for example, had to be changed to reduce the need to enter and exit the room and better preserve already scarce PPE.
“I’m very proud of my team. They adapted so quickly to COVID-19. It was like, ‘This is what we’ve trained for, and it stinks, and we’re scared, but this is what we’re going to do.’ And they did it. They did it,” emphasizes Baudin.
Because of nursing’s response, Baudin feels validated that the simulation and hands-on training they conduct in the SPU is effective and more necessary than ever before. Even as Boston still grapples with COVID-19, preparing and training for the next viral assault will continue at the SPU. Now the unit is strengthened by an army of nurses who have experienced the hot zone firsthand.