How Boston Health Care for the Homeless Is Successfully Vaccinating Shelter Guests
March 25, 2021
By Meryl Bailey
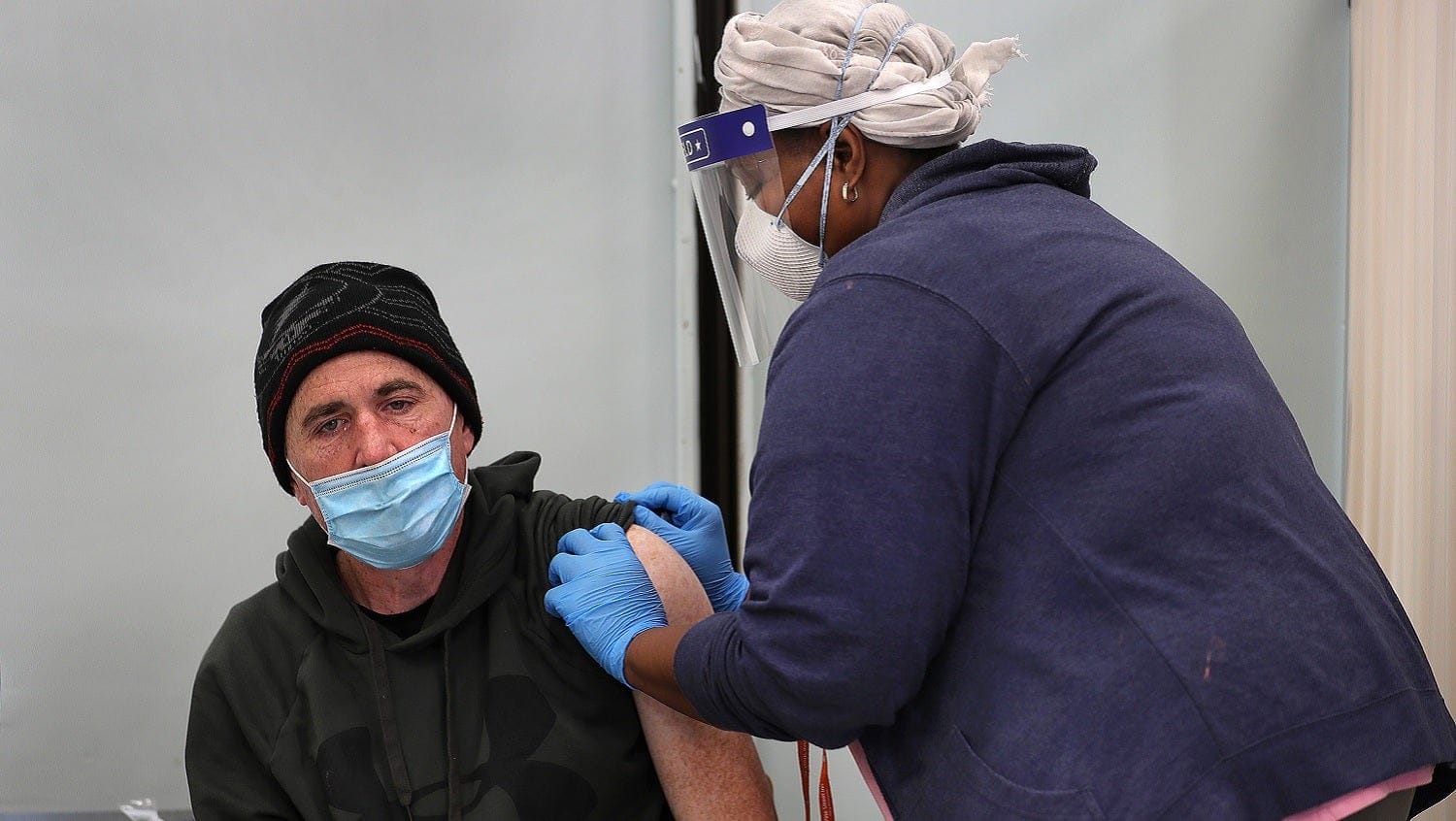
Boston Globe, Getty Images
Boston Health Care for the Homeless Program is vaccinating people in shelters who often have mental health comorbidities. Trust is key.
The impact of COVID-19 on people experiencing homelessness has been deeply concerning to public health officials since the beginning of the pandemic a year ago. The close confines of congregate shelter settings coupled with the severe comorbidities of many in the homeless population make this group particularly susceptible to contracting COVID-19 and suffering from the most severe infection. Boston Health Care for the Homeless Program Medical Director Denise De Las Nueces says as many as 40% of guests had COVID-19 in some of the largest shelter settings during the first wave of outbreaks before Boston decanted shelters in the spring and summer of 2020 and isolated infected individuals.
A successful vaccination rollout in the homeless shelter system is key to curbing the spread of COVID-19, but health providers face many barriers to achieving their goal. Effectively communicating the new vaccine’s facts across languages and cultures and easing concerns that lead to vaccine hesitancy is of top priority — especially in a patient population with so many social and economic vulnerabilities. The effort has wide-ranging implications that include an impact on individual health, preventing emerging variants, and easing the strain of serious infections entering the city’s hospital systems.
The importance of trusted healthcare sources in the vaccine rollout
Staff at the Boston Health Care for the Homeless Program (BCHCP), in concert with city health officials and community partners, have put COVID-19 vaccine shots into the arms of more than 2,300 guests and staff of area homeless shelters since the Commonwealth’s phase one rollout began in January. This number surpasses the one-half mark in the organization’s massive effort to fully vaccinate 3,500 shelter staff and guests who became eligible during the first wave of vaccinations. Of the staff and guests that have received their first dose of vaccine, 20% are Latinx and 38% are Black — encouraging numbers considering worries over heightened vaccine hesitancy among people of color.
BHCHP has a 30-year history working on the ground to provide healthcare to people in Boston who chronically experience homelessness. The clinical team’s longtime presence embedded in shelter settings has helped build trust within the community, which has been critical for past mass vaccination efforts. De Las Nueces, who is also an assistant professor of medicine at Boston University School of Medicine, notes that BHCHP was on the frontlines during a deadly outbreak of meningococcal disease in 2016 and provided successful outreach that is informing their COVID-19 vaccination rollout.
“In 2016, we had to really quickly launch a meningococcal disease vaccine campaign. In two-months’ time, we vaccinated more people against meningitis than we had the previous two flu seasons,” she explains. “We had great success in that effort and subsequent efforts around smaller outbreaks. And so, I think that is demonstrative of the fact that we were starting with a really good foundation of preexisting trust among our patient population.”
Understanding the homeless population’s unique vaccine fears
In preparation for phase one COVID-19 vaccinations, BHCHP surveyed shelters to identify staff’s top vaccine concerns and produced multilingual health education to better inform the culturally diverse populations working and residing in shelters.
Concerns over the speed of the development of the new vaccines, the mRNA technology used in Pfizer-BioNTech and Moderna formulas, and worries over being first in line to receive immunizations are nearly universal. However, De Las Nueces and her colleague, BHCHP Chief Equity Officer Sonja Spears, note the team must also address unique fears. Many in their patient population struggle with severe mental illness, including paranoia, heightening anxiety and fears around vaccinations. Feelings of powerlessness over coercion are also prevalent.
“Something that we heard from some of our patients is the fear that they might be coerced into getting the vaccine in order to be allowed access to places like shelters, public facilities, and city transportation,” says Spears. “Considering that very often people that are experiencing homelessness are stigmatized and barred or banned access or have to face restricted access for many places, this was something that was of real concern to them.”
Both De Las Nueces and Spears underline the importance of human-centered outreach from providers and people who truly understand the barriers this population faces.
As a result of learning and understanding the population’s unique concerns and hesitance, BHCHP is working with shelters to identify COVID-19 vaccine ambassadors. Ambassadors are guests of shelters who chose to receive the vaccine and are willing to speak to concerned individuals about their experience. Ambassadors will receive training from BHCHP to help further provide accurate information about vaccines and will receive a $5 gift card for their time.
The new program started at the end of February, but already the response has been strong. Spears hopes that partnering with individuals who have lived experience with homelessness will further ease concerns of the COVID-19 vaccination effort.
Using data for second-dose adherence and future care
BHCHP providers are currently using the Moderna vaccine, which requires a 28-day wait period between doses. Second-dose vaccinations started at the end of February, and De Las Nueces is pleased by the number of patients adhering to protocol. They had estimated in early March that about two-thirds of those eligible would receive their second shot, however, new data shows that 77% of guests completed two doses on their appointment date — a statistic De Las Nueces calls “astounding.”
Patients receiving vaccines are tracked through the shelter system’s Homeless Management Information System, helping alert health providers to patients who move between shelters and are due for their second dose.
“What we were really happy to see is that for those second-dose clinics, there was also a bolus of people walking in for their first doses. So, people, presumably based on the experience of peers, maybe people who were reluctant to be the first adopters, but after a month’s worth of efforts and seeing how their peers have experienced the vaccine now feel more comfortable being vaccinated. So that was nice to see,” she says.
Spears notes the team is also using data collected from the vaccination effort to inform future care.
“Our efforts around health equity are forward-looking as well,” Spears says. “During the distribution and administration of the vaccine, we’re making sure that we collect data that is accurate so that we will be able to have more information going forward that will make our efforts smoother and more targeted for the populations we are serving.”
Where BHCHP’s vaccine rollout stands now
BHCHP is currently working to reach patients eligible in phase two of the state’s rollout, including individuals age 60 and older and those with two or more comorbidities as specified by the state. Due to the high prevalence of tri-morbid disease — significant chronic medical conditions, severe mental illness, as well as substance use disorders — many individuals unconnected with the shelter system and living on the street likely qualify for vaccination in phase two.
Currently, the BHCHP team is reaching out to eligible people through its mobile van unit, through a partnership with street outreach teams, and the brick-and-mortar BHCHP medical offices.
The newly approved Johnson & Johnson vaccine, which can be administered in one dose and has less stringent storage requirements, will hopefully accelerate BHCHP’s vaccination efforts both in the shelters and more broadly to unhoused individuals in subsequent phases.
As that effort moves forward, BHCHP continues to work collaboratively with the medical field, social service agencies, and municipal partners to reach eligible patients.
Ultimately the success of the effort comes down to earnestly building trust.
“We have been meeting people where they are and making sure that they have accurate information in their primary language that is culturally sensitive,” emphasized De Las Nueces. “Then we allow them to make the decision without any judgment attached. I think that is the most important thing, and it feels intuitive to us.”