HPV-Linked Throat Cancer Is Preventable. This Clinic Offers the Vaccine and Awareness.
October 14, 2021
By Meryl Bailey
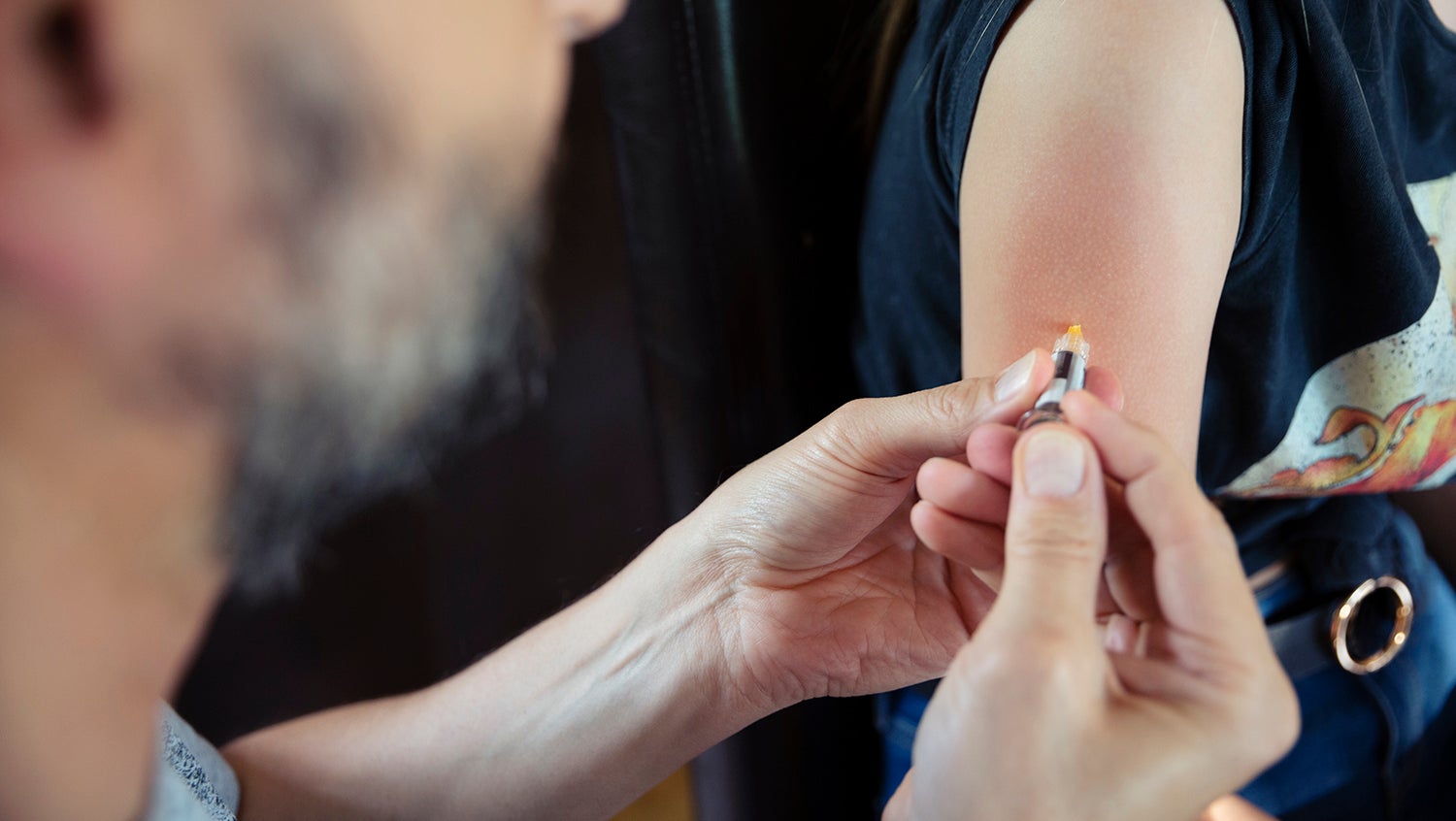
Getty Images
BMC’s innovative clinic provides same-day shots and a chance to research barriers to vaccination.
Human papillomavirus, or HPV, is the most common sexually transmitted disease and probably best known as the leading cause of cervical cancer. Thanks to increased awareness, preventive screenings, and the introduction of an HPV vaccine in 2006, the incidence of new cervical cancer has declined in the U.S. Unfortunately, other HPV-positive cancers are on the rise.
Oropharyngeal cancer, commonly known as throat cancer, is now the leading cancer caused by HPV. It’s a cancer that predominately affects men, and there is little public awareness about it or its prevention.
As a head and neck surgical oncologist specializing in HPV-related cancers, Daniel Faden, MD, sees how destructive oropharyngeal cancer can be. Aside from the life-threatening cancer itself, treatment for HPV-positive oropharyngeal tumors has profound effects on daily life and function, affecting speech and swallowing, and negatively impacting quality of life. What’s especially tragic is that HPV-positive throat cancers in both men and women are preventable with a vaccine.
In 2020, the FDA specifically approved the use of Gardisil 9 for the prevention of oropharyngeal cancers in men aged 9 through 45. The FDA’s announcement—combined with the rising rate of these cancers, low vaccination rates, and a general lack of knowledge regarding the relationship between HPV and throat cancer—prompted Faden and a team of physicians and nurses at BMC’s Department of Otolaryngology-Head and Neck Surgery to set up a pilot point-of-care HPV vaccination clinic to help improve immunization rates.
“At the current rate of vaccination, we’re really not going to have an impact on even this generation in terms of preventing development of head and neck cancers. There is a large percentage of the population who may benefit from being vaccinated but currently isn’t vaccinated,” says Faden, underlining the urgent need to understand the gaps in care that are leading to this disparity.
An innovative HPV vaccine clinic that’s both research and intervention
Part research project, part intervention, the HPV vaccine clinic is the first of its kind to be housed in an otolaryngology department. Faden hopes to measure the awareness people have about HPV-related cancers, gain insight on why some patients are not vaccinated, and understand the barriers to vaccination.
All patients are asked to complete a survey to assess their knowledge about HPV, the HPV vaccine, and the relationship between HPV and head and neck cancers.
The last question on the survey asks, “If you qualify for vaccination, would you want to receive a vaccine today?” If a patient chooses yes, they are offered an appointment that day to discuss the vaccine, assess if they qualify, and deliver the vaccination at that time.
Not everyone is a good candidate for the vaccine, however, notes Faden—especially adults in long-term monogamous relationships. The vaccine is most effective when given before the initiation of sexual activity and exposure to HPV, which is why boys and girls are recommended by their pediatrician to receive it at age 11 or 12. However, in some cases, adults up to the age of 45 can still benefit. Results from Faden’s study suggest a significant portion of BMC’s patient population qualify for vaccination but are not vaccinated or have not completed the series.
“Access to care is definitely an issue for BMC’s patient population. For example, if you’re an immigrant to the United States, you may not have had the opportunity to be vaccinated earlier in life,” he says. “Depending on health literacy levels and general access to care, certain groups are more under-vaccinated.”
‘An ounce of prevention is worth a pound of cure’ for HPV
So far, Faden is encouraged by the number of patients interested in vaccination. The department is vaccinating about 10% of participants who fill out the survey—higher than what they anticipated.
The research team is now analyzing the survey responses to understand what barriers exist to vaccination and will then design interventions to help overcome these barriers. Ultimately, the goal is to protect more people from developing cancer by making the vaccine more accessible to those eligible. To a surgeon who spends his days on the front lines of cancer treatment, the old adage “an ounce of prevention is worth a pound of cure,” rings particularly true.
“Vaccinating patients may potentially completely abrogate the development of a cancer later in life, which is amazing to think about, right?” Faden says. “I spend my career researching the molecular underpinnings of HPV-related head and neck cancers so we can better treat patients who already have cancer, when we could just prevent them from getting it in the first place by giving them a few painless shots.”


