New Strategies Confront the Critical Need to Improve Sickle Cell Disease Care
April 12, 2021
By Meryl Bailey
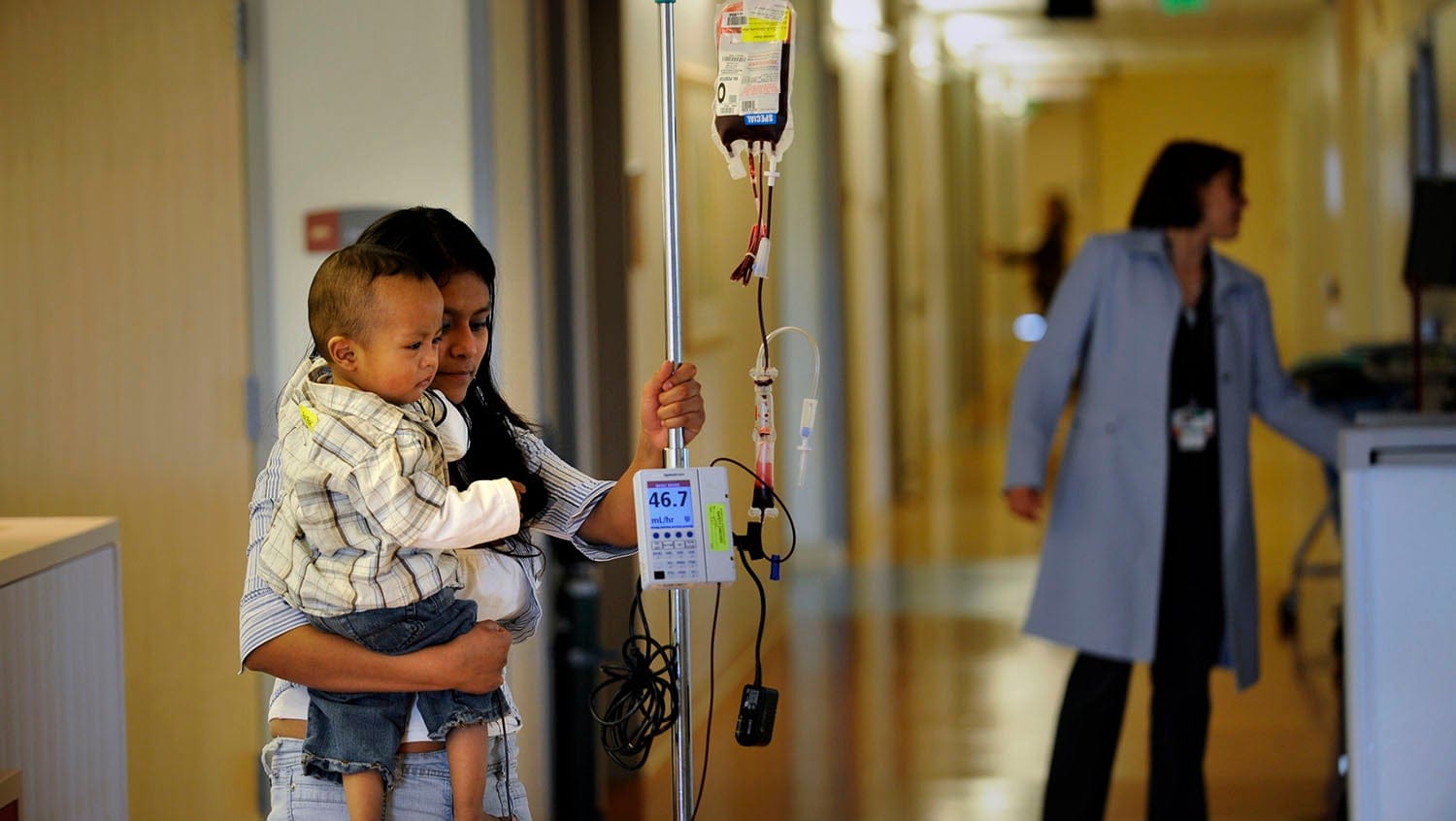
Denver Post, Getty Images
Progress toward improving outcomes for adults with sickle cell disease hinges on more qualified, trained physicians and investment in longitudinal research.
Universal newborn screening and early treatment mean 90% of Americans born with sickle cell disease (SCD) will live to adulthood. However, few adult physicians understand how to treat the complex, chronic nature of this rare disease, and still too little is known about its progression over time — resulting in a survival rate for adults with SCD that has changed little over 40 years. As a historically underfunded disease that primarily affects people with African ancestry, the medical community is confronting the long history of institutional racism that has hindered advancements in care.
Recently, the National Academies of Sciences, Engineering, and Medicine (NASEM) released a strategic plan to improve care for sickle cell disease, which includes calls to increase the physician workforce and further research.
“It is a national emergency. There is a national shortage of physicians in any specialty, including hematology and primary care, trained and qualified to care for patients with sickle cell disease,” says Elizabeth Klings, MD, director of the Center for Excellence in Sickle Cell Disease at Boston Medical Center (BMC). “We have not matched the fact that we’ve improved survival to adulthood with increasing the adult physician workforce. It is a major healthcare disparity for patients.”
BMC’s Center for Excellence in Sickle Cell Disease is the largest specialty center in New England, with a multidisciplinary team that cares for 450 patients annually from newborn to adulthood. Thanks to a seed grant of $250,000 from the Vela Foundation, the Center is embarking on two new initiatives to improve care for adults with SCD: a new advanced fellowship and an SCD biospecimen bank. Both initiatives address critical needs outlined in the NASEM report to help reduce health disparities for people living with SCD.
Advanced fellowship to improve sickle cell disease care
An estimated 100,000 Americans live with SCD. Considered an “orphan” disease by the National Institutes of Health, SCD has received little federal funding to further research, which has disincentivized clinician investigators from pursuing the field. The critical shortage of adult physicians with expertise in SCD means people confront a medical system unprepared to handle their complex needs, including hospitalization for acute chest syndrome and severe pain episodes due to vaso-occlusive crises. Patients frequently confront bias, discrimination, and delayed treatment when seeking care.
The first of its kind in the country, BMC’s new one-year SCD advanced fellowship will develop clinician investigators with expertise in sickle cell disease that extends beyond traditional training programs. Klings underscores the essential need to offer advanced training in the field.
“Traditionally, physicians who take care of adult patients with sickle cell disease are either trained in hematology or oncology or hematology and adult internal medicine. Many of these programs lack training focused around sickle cell disease, and many graduates of these training programs leave their program feeling unqualified to take on the care of patients with sickle cell disease,” she explains. “Our goals for the trainee over the year of the fellowship is to establish a clinical and research footprint in sickle cell disease so they can begin to be able to develop a career in sickle cell disease as a clinician investigator.”
Biospecimen bank to further longitudinal SCD research
Scientific investigation of SCD has advanced breakthroughs in the understanding of genetic diseases and hematology, yet, until recently, there have been few innovations in approved treatments for the painful inherited blood disorder. Over the past two years, therapeutics for the disease have doubled, with four approved treatments now available to treat this disease and its complications.
A major obstacle in advancing the treatment of patients with sickle cell disease has been a lack of understanding of biomarkers to help guide treatment decisions and provide insights on potential new therapeutic targets. The ability to link biospecimens to clinical information in patients with SCD is critical to advancing the understanding of the natural history of the disease and the optimal use of currently available therapies and in the development of novel treatment strategies.
“The biobank will allow us to utilize our wealth of clinical material as the largest sickle cell center in New England, which has a patient population that spans the lifespan from birth to death. Cataloging and studying these samples will allow us to conduct genetic studies, biomarker studies, and other research that may help yield insights into disease pathogenesis and the response to newer therapies, especially when used in combination,” explains Klings.
Patients’ willingness to donate samples to the biobank remains an open question, but Klings believes the recent approvals in therapeutics to treat SCD will encourage her patients’ future enrollment in clinical trials at BMC.
“Our patients understand that their disease has been understudied for years. They have also experienced care from physicians and other members of the healthcare community who have an incomplete understanding of their disease. There is a lot of interest from the community in trying to change that in any way possible, and I expect that our patients are going to be very interested in participating,” she says.


