One Patient’s Journey Underscored Inequities in Ear, Nose, and Throat Health
October 19, 2021
By David Limm
Getty Images
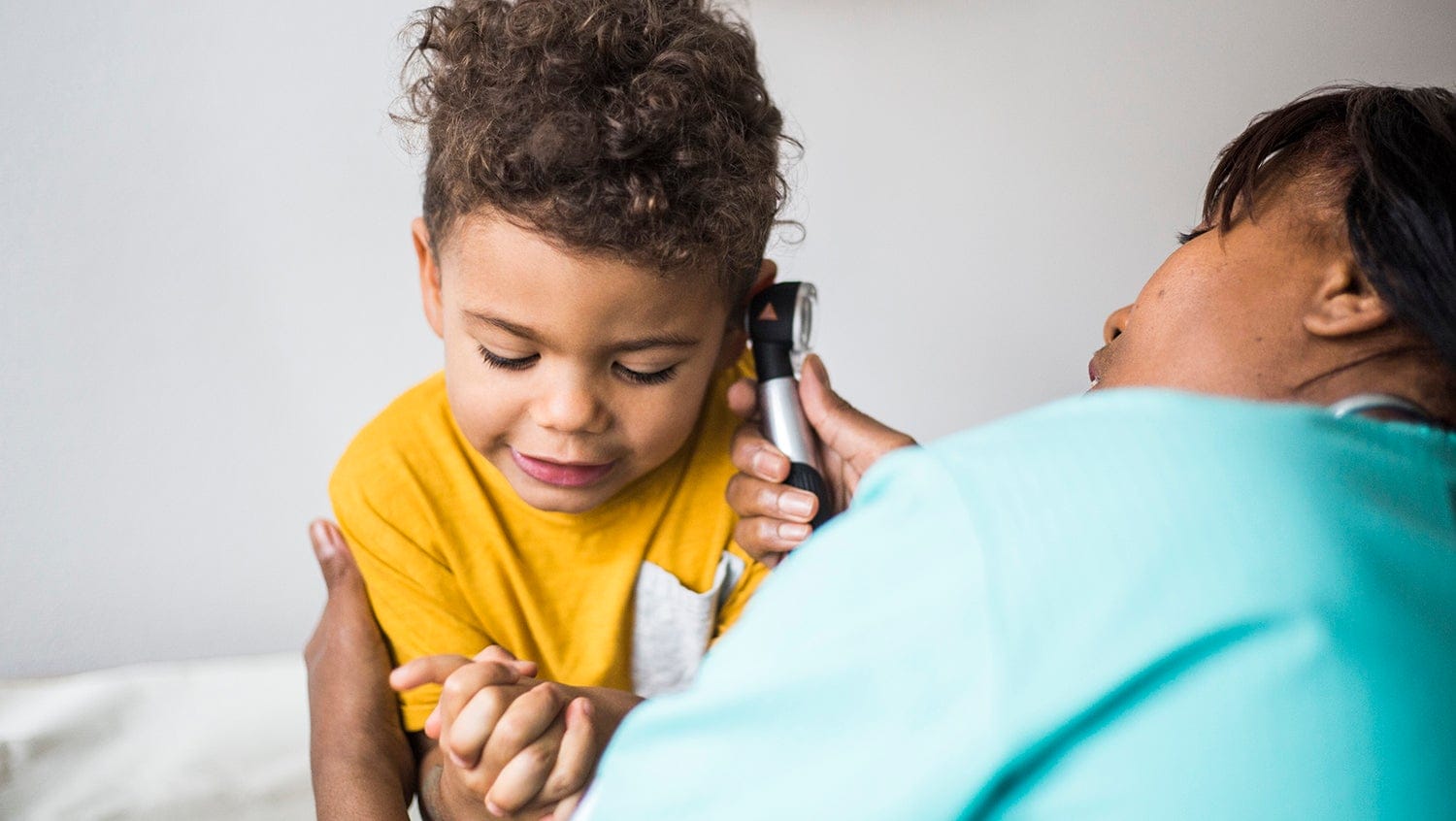
BMC resident Joseph Sabra, who treated the patient, says otolaryngologists must study social determinants of health that create barriers to care.
In 2017, researchers analyzed National Health Interview Survey data and found that Black and Hispanic children are less likely to be identified or diagnosed with common pediatric otolaryngological conditions like frequent ear infections, hay fever, sinusitis, and strep pharyngitis than white children.
Black and Hispanic patients are also significantly less likely to visit an outpatient otolaryngologist than white ones, according to a study about racial gaps in the utilization and cost of care.
At a virtual meeting of the New England Otolaryngological Society this month, third-year Boston Medical Center (BMC) resident Joseph Sabra, MD, addressed these and other racial, ethnic, and socioeconomic disparities that children in the U.S. face when it comes to ear, nose, and throat health.
Health outcomes haven’t matched healthcare spending, Sabra said, because there hasn’t been enough investment in public health measures that focus on social determinants of health.
While he reinforced BMC’s track record of studying and addressing root causes and its commitment to providing consistent, accessible health services to all patients, he emphasized that there was far more work to be done.
“It is clear that more investigation into this topic is needed in the future,” he said. “So the question is: Where are we now, and where are we going in the future?”
To illustrate his point, Sabra recounted the story of a memorable otolaryngology patient he once treated.

Joseph Sabra, MD
“As I think about Boston Medical Center’s mission to provide consistent, accessible health services to all patients who come through its doors, I think of one incredible patient I had the pleasure of treating during my intern year.
This gentleman immigrated to Boston from outside the United States to seek medical care. Three days after he arrived in the United States, he walked into the Emergency Department at Boston Medical Center. He reported that he had three prior operations in his country for treatment of a posterior neck mass over the past 18 years. He was told that it was not cancer, and each time after surgery it grew back larger. He was in significant pain and was seeking a definitive treatment.
The patient underwent a wide local excision of the mass with removal of the outer table of the occipital calvarium as well as the spinous processes of cervical vertebrae with posterolateral neck dissection, local advancement flaps as well as a latissimus pedicled muscle flap and split thickness skin graft. Unfortunately, he developed an infection that compromised the muscle flap, requiring flap takedown, and multiple washouts and debridements. He was offered integra matrix and wound vac assisted closure of this area, and ultimately a second split thickness skin graft. Final pathology was consistent with a cutaneous squamous cell carcinoma.
Observing this patient’s journey, going through 18 years of suffering due to poor access to quality medical care, highlights how the social determinants of health can impact our patient populations…
There have been multiple studies published in the past few years that elucidate how prevalent health disparities are in the field of otolaryngology.
Rotsides et al, sought to investigate differences in epidemiology of oropharyngeal squamous cell carcinoma with regards to human papillomavirus, race, and socioeconomic status using the national cancer database. [Nearly 46,000] patients met the criteria for the study. They found that significant differences in HPV status exist between socioeconomic and racial groups, with HPV negative disease more common among Black patients in lower socioeconomic status groups…
The striking difference in this investigation is that even when controlling for HPV status, Black race and lower socioeconomic status was still associated with worse survival of oropharyngeal squamous cell carcinoma…
We, as otolaryngologists, must continue to be cognizant of the barriers our patients are facing and continue our efforts to help them to overcome the obstacles to quality healthcare.“
The above is an edited excerpt from Joseph Sabra’s presentation to the New England Otolaryngological Society’s virtual event on Oct. 8, 2021.


