Epidemics at Odds: Preventing the Next Wave of the Opioid Crisis During COVID-19
March 23, 2020
By Dave Wedge
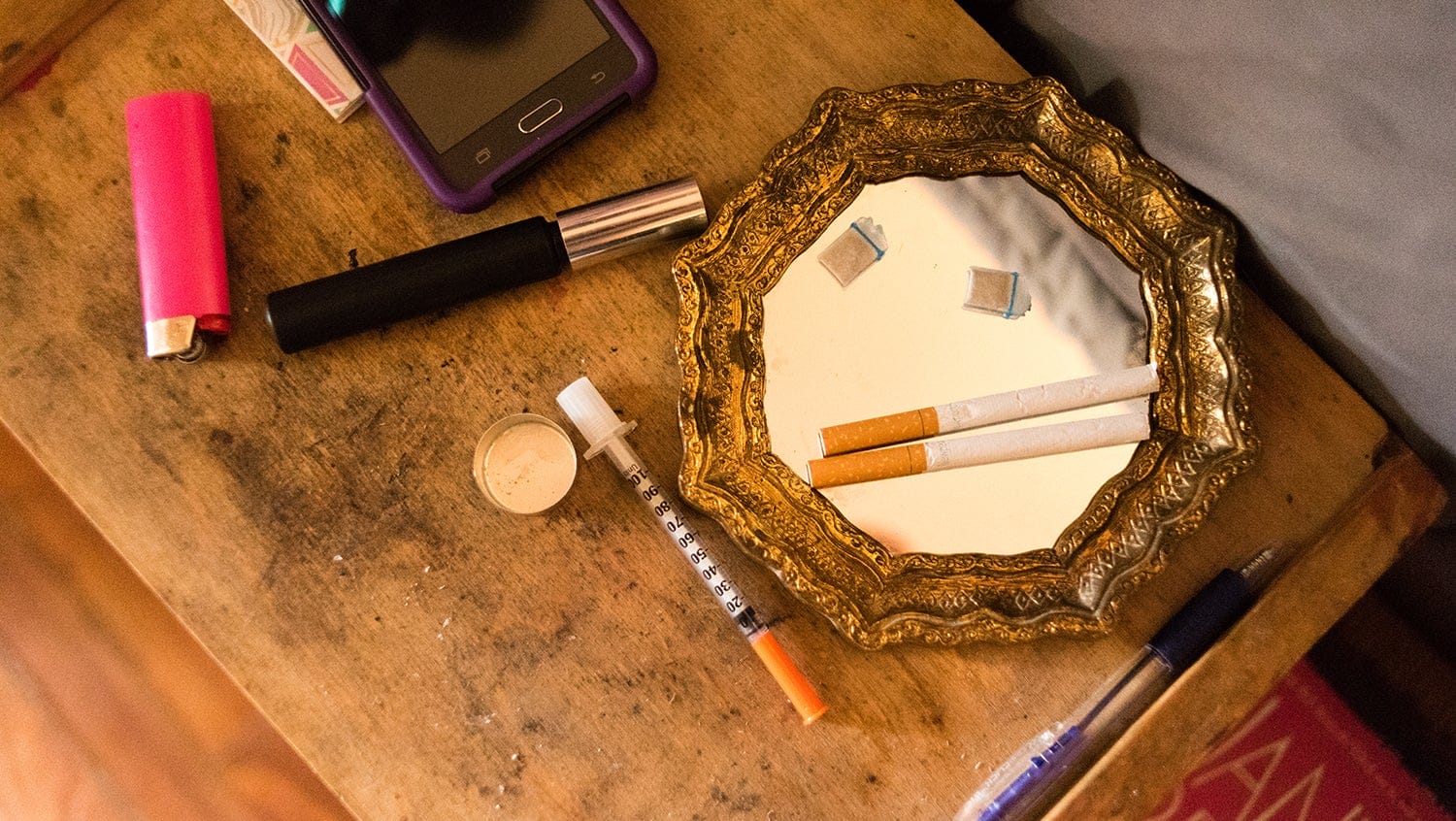
Getty Images
Addiction expert Miriam Komaromy, MD offers a frank look at the opioid epidemic and shares how efforts are underway to keep crucial care accessible.
As COVID-19 cases increase and patients displace those being treated for other conditions at hospitals and medical centers across the country, there is growing concern that the virus will have far-reaching impacts on our healthcare system. Among them are the hindered delivery and success of substance use treatment. Experts remind us that mere weeks ago, the opioid epidemic was the biggest health concern in our country — and it’s still here, with patients and providers alike facing new serious challenges.
The evolving situation is raising concerns that heightened anxiety may push people out of recovery. Lockdowns and decreased access to treatment centers due to social distancing is likely to disrupt distribution of crucial treatment medications. And all of it boils down to the real potential for a surge in overdoses and overdose deaths.
Bold and innovative steps are being taken, however, to address these and the many other complex addiction issues emerging because of the coronavirus pandemic. Miriam Komaromy, MD, the medical director of the Grayken Center for Addiction at Boston Medical Center (BMC), her staff, and partner organizations are devising a comprehensive strategy to maintain substance use disorder treatment services in the face of COVID-19.
A Fulbright Scholar who joined BMC in August 2019, Komaromy is one of the nation’s leading clinical educators for addiction medicine. She spoke with HealthCity about the anticipated impact the coronavirus crisis will have on the addiction and recovery community, the challenges treatment providers are expected to face, and how the Grayken Center is preparing to continue delivering effective services to those who need it most.
HealthCity: What impact do you foresee as treatment beds are lost to make room for patients with COVID-19?
Miriam Komaromy, MD: The COVID-19 infection, pneumonias, and other problems, are kind of like a monster that’s going to be chewing up the healthcare system bit by bit. There will be decreasing access to all kinds of care. We’re particularly focused on trying to find ways to ensure that patients with substance use disorders can still get treated because we desperately want to avoid a next-wave epidemic of relapse and overdose following this.
HealthCity: Do you think there could be a surge in overdoses in the coming weeks and months?
MK: I do, yes. And I think that our providers here in Boston are recognizing that. Outreach efforts are being geared up to provide overdose prevention education, increase syringe exchange, and engage patients in treatment. Patients who are homeless and have substance use disorders have such incredibly stressful lives already — adding in the stress of this infection may well push some people who are in or getting into recovery into relapse. We need to be prepared to offer services to those folks and try and help them avoid just spiraling.
HealthCity: How well is Boston prepared to handle these complex public health issues?
MK: The services that we have here are actually quite well-developed compared to what’s available in a lot of the country, and we’re probably as prepared as anybody to mount a public health response and support vulnerable populations. I’m really confident that the efforts that we’re making are going to pay off and are going to help to limit the spread.
HealthCity: How are providers and the city collaborating to prevent the worst-case scenario?
MK: We’re working to help support the tents that Boston Health Care for the Homeless is putting up in collaboration with the City of Boston to isolate or quarantine patients who lack housing, for example. Significant numbers of those patients are going to be people who have substance use disorders that can be treated medically. They might be in danger of experiencing alcohol withdrawal if they go into one of those tents and are kept there. They might have untreated opioid use disorder or they might not be able to get out to get their medications.
So we’re trying to make sure that we have staff available to do video telehealth interactions with those patients. And for all patients who we connect with — either face-to-face or virtually — we’re trying to prescribe longer prescriptions to decrease the need for contact and the need for people to go out and get prescriptions.
HealthCity: Have any challenges emerged as you’ve moved to more telehealth-based care?
MK: One issue we’ve been working to understand is telehealth prescribing of buprenorphine, which is being allowed over a lot of different platforms, some of which may or may not be HIPAA compliant. Someone might need to talk to their medical provider over FaceTime or Skype, but those aren’t HIPAA compliant platforms. So, we need to evaluate risk versus benefit. And when we weigh potential overdose death against a remote chance of loss of personal privacy, it seems clear that relaxing the privacy rules in this epidemic was the right thing for the federal government to do.
HealthCity: Do you expect this disruption will exacerbate racial and other social disparities in who receives treatment for substance use disorder?
MK: COVID-19 is shining a glaring spotlight on those kinds of inequities and disparities in our population. So many people in our country live one paycheck away from economic disaster. The pain and the impact is going to be most severe on people who are already socially vulnerable.
The homeless population and the population with substance use disorders are at increased medical risk because of increased rates of chronic medical illness and decreased access to care and services. I’m afraid this is going to worsen those kinds of disparities and have a disproportionately harsh effect on the most vulnerable people in our society.
HealthCity: Do you think these problems make an even stronger case for systemic changes?
MK: The case is being made very clearly for universal health insurance. When we are not taking good care of our most vulnerable patients, they are tipped into worsened health. That increases cost on the healthcare system and overburdens it. It doesn’t just affect the people who have limited access, it affects all of us. If we’re not taking care of people who are living in the most crowded and vulnerable conditions, they’re at hugely increased risk. But the rest of us are also going to feel that risk echoing out through society.
Let’s do the right thing now, while we can, and get the most vulnerable members of our society off of the street and into housing. We will decrease their risk and in turn we will decrease the risk for society.
This interview has been edited and condensed.